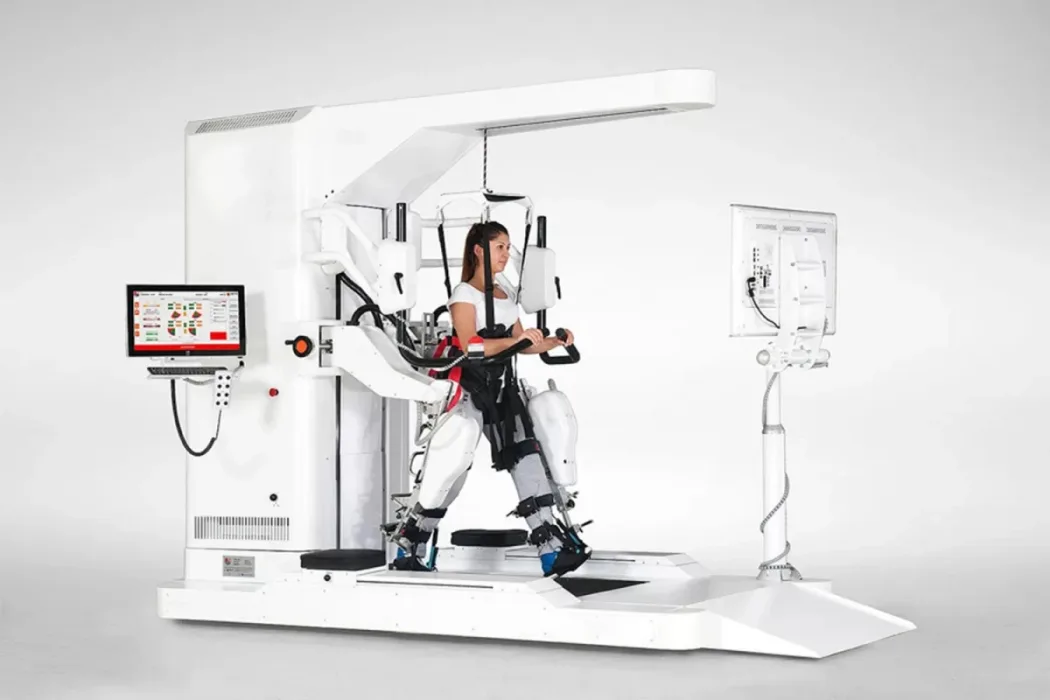
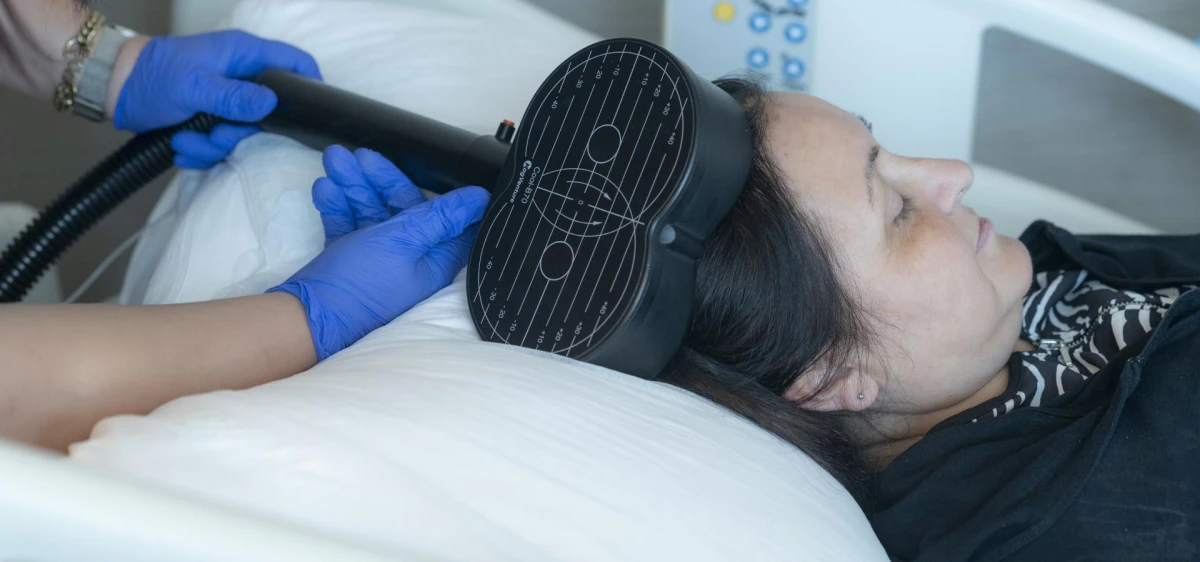
Using Robotic and Conventional Rehabilitation Together in Stroke Rehabilitation
In recent years, the integration of robotic devices into rehabilitation processes has been considered an important development for both patients and healthcare professionals. Especially after neurological conditions such as stroke, brain injury, and spinal cord injury, the availability of high-repetition and intensive exercises through robotic systems has increased accessibility and generated great interest in this field. However, this growing excitement also brings an important risk: seeing technology as the treatment itself.
Observations from clinical practice show that technological advancements can sometimes overshadow the real goals of therapy. In reality, robotic devices are tools of therapy, not its purpose, similar to parallel bars or resistance bands used in conventional rehabilitation. Unfortunately, in some cases the focus shifts to what the robot is doing rather than why the patient is performing a movement. This approach can disrupt one of the core principles of motor learning: purposeful and meaningful movement production.
Below are some common mistakes encountered in robotic rehabilitation:
1. The presence of the device replaces the therapeutic goal
Simply using a robotic device does not automatically make a therapy session effective. Repetitions without a clear purpose may produce movement but do not necessarily reshape the brain. For example, collecting virtual objects in a robotic therapy game may have limited functional benefit if it does not relate to the patient’s real-life needs.
2. The same robot and protocol are used for every patient
Robotic rehabilitation must be individualized. Applying the same device and the same protocol to patients with different functional limitations—such as difficulty grasping objects versus difficulty releasing them—may be inefficient and a waste of valuable therapy time. The selection of robotic exercises and games should be carefully planned by therapists according to each patient’s needs.
3. Passive applications are considered sufficient
Robotic systems often assist patient movement, which can be beneficial for individuals with very limited mobility. However, if the robot performs most of the movement passively, active participation and patient effort may decrease. Therapy sessions where the patient does not actively contribute may appear effective in the short term but often fail to produce lasting functional improvements.
4. The therapist’s planning role is overlooked
In some situations, the automated exercise options or pre-programmed protocols offered by robotic systems may overshadow the therapist’s clinical decision-making process. However, it is important to remember that a robot is not a therapist. The therapist determines which patient should use which device, with what intensity, and for what therapeutic goal. The robot simply supports this process.
What Should an Effective Robotic Rehabilitation Session Look Like?
Considering the limitations described above, several fundamental principles can guide an effective and patient-centered robotic rehabilitation session:
- Work with meaningful goals: Exercises should be directly related to the patient’s daily life activities, and each movement should have a clear purpose.
- Individualize treatment: The selected robotic device, exercise content, and intensity should be tailored to the patient’s functional condition and rehabilitation needs.
- Encourage active patient participation: The robot should not completely take over the movement; instead, the patient should be encouraged to actively contribute and exert effort.
- Technology should be guided by the therapist: Robotic systems should support clinical decision-making rather than replace it. Clinical evaluation—not automated protocols—should guide the therapy process.
It should be remembered:
Robots can contribute to meaningful and lasting recovery only when they are combined with appropriate therapeutic goals. Technology should serve patient-centered rehabilitation rather than replace it.